Veren biomarkkerit ovat ratkaisevia arvioitaessa yksilön yleistä terveyttä ja pitkäikäisyyttä. Vaikka jokaisen biomarkkerin merkitys voi vaihdella henkilön iän, sukupuolen, sairaushistorian ja yleisen terveydentilan mukaan, on olemassa 45 välttämätöntä veren biomarkkeria, joita käytetään yleisesti terveyden ja pitkäikäisyyden indikaattoreina nykyisen tieteellisen tiedon perusteella.
On tärkeää huomata, että vaikka veren biomarkkerien testaus on hyvä alku, se ei ole ainoa tapa mitata terveyttä ja pitkäikäisyyttä. Muita testejä ja markkereita, jotka voivat antaa kattavamman kuvan terveydestä ja pitkäikäisyydestä, ovat orgaanisten happojen testi , joka mittaa ravitsemuksellisia ja metabolisia biomarkkereita sekä virtsan aminohappojen ja veren rasvahappojen määrää. Lisäksi mikrobiotan ja mikrobiomin kvantifiointi voi tarjota olennaista tietoa suoliston terveydestä ja sen vaikutuksista yleiseen terveyteen.
Lisäksi laadukas ja kattava geneettinen testi (DNA) voi antaa tietoa yksilön geneettisestä rakenteesta ja mahdollisista geneettisistä taipumuksista tiettyihin sairauksiin. Epigeneettinen testi voi myös antaa tietoa siitä, kuinka elämäntapa- ja ympäristötekijät vaikuttavat geenien ilmentymiseen ja mahdollisiin terveysvaikutuksiin. Siksi on ratkaisevan tärkeää harkita näiden testien ja merkkien yhdistämistä saadaksesi täydellisen kuvan yksilön terveydestä ja pitkäikäisyydestä.
Johdanto
Lääkärit pitävät löydöksiä yleensä "normaaleina", jos ne ovat vertailualueella. Usein he kaipaavat kokonaiskuvaa jättämällä huomioimatta erilaisia merkkejä. Vertailualueella olevaa testitulosta pidetään "normaalina". Lääketieteellinen laboratoriotiede sijoittaa sanan kuitenkin lainausmerkkeihin, koska normaalin ja epätavan välillä ei ole selkeää rajaa. Tästä syystä termiä "viitealue" käytetään "normaalin alueen" sijaan.
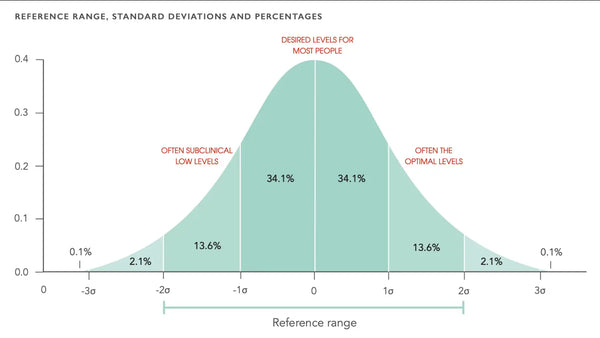
Laboratoriotulos voi olla hieman korkeampi tai pienempi kuin vertailualue, mutta se ei viittaa siihen, että henkilö on sairas. Tämä on ongelmallista hyvän terveyden ylläpitämisen ja sairauksien ehkäisyn kannalta. Yllä oleva tulkinta on epäilemättä oikea, jos terveyttä tarkastellaan yksinkertaisesti sairauden puuttumisena. Kuitenkin, jos terveyttä pidetään elinvoimaisena ja hyvänä väestö- ja yksilötasolla, vertailualuetta voidaan tarkastella eri tavalla.
WHO (Maailman terveysjärjestö) otti kantaa tähän aiheeseen lausunnossaan vuodelta 2014; Heidän viimeisimmässä kattavassa raportissaan, joka julkaistiin International Journal of Epidemiology -lehdessä vuonna 2016, todettiin "terveys ei ole vain sairauden puuttumista...". Kansainvälinen ymmärrys tästä on viime aikoina lisääntynyt ja ennaltaehkäisevästä terveydenhoidosta on tulossa yhtä tärkeä alue sairauksien sairaanhoitoon verrattuna.
Mikä on optimaalinen taso?
Kaikilla laboratoriomarkkereilla ei tietenkään ole tieteellisissä tutkimuksissa määritettyjä ns. optimaalisia arvoja, mutta sellaisia on joissain tapauksissa olemassa. Optimaaliset arvot perustuvat todennäköisesti populaatiotasolla tehtyihin löydöksiin alhaisesta kuolleisuudesta tai esimerkiksi suurimmasta todennäköisyydestä ehkäistä tiettyyn markkeriin liittyvää sydän- ja verisuonitautia. Joillekin vitamiineille on myös määritelty optimaaliset tasot, toisin kuin vertailualue. Esimerkiksi testosteronitaso vertailualueen alemmalla tasolla voi viitata subkliiniseen hypogonadismiin .
On kuitenkin tärkeää aina verrata tuloksia aikaisempiin tuloksiisi ja seurata muutoksia ajan myötä, erityisesti elämäntapamuutosten jälkeen. On myös hyödyllistä ottaa useita näytteitä, jotta saadaan isompi kuva eri tasoista ja minimoida pientä päivittäistä vaihtelua ennen tulosten tulkintaa.
45 tärkeintä veren biomarkkeria
On olemassa lukuisia veren biomarkkereita, jotka ovat tärkeitä terveydelle ja pitkäikäisyydelle, ja niiden merkitys voi vaihdella riippuen henkilön iästä, sukupuolesta, sairaushistoriasta ja yleisestä terveydentilasta. Nykyisen tieteellisen tiedon perusteella tässä on kuitenkin luettelo 45 veren biomarkkerista, jotka on luokiteltu ilman erityistä järjestystä ja joita käytetään yleisesti terveyden ja pitkäikäisyyden indikaattoreina .
On tärkeää huomata, että biomarkkereita ei pidä tulkita erillään, ja niitä tulee aina tarkastella yksilön sairaushistorian, elämäntapatekijöiden ja muiden asiaankuuluvien terveysmittareiden yhteydessä (kaikki viittaukset merkkiaineisiin ja muihin löytyy Optimoi Laboratoriotulosten verkkokurssi ).
- C-reaktiivinen proteiini (CRP): CRP on proteiini, joka lisääntyy vasteena kehon tulehdukselle. Korkeat CRP-tasot on yhdistetty lisääntyneeseen sydänsairauksien, diabeteksen ja muiden kroonisten terveyssairauksien ja kuolleisuuden riskiin. CRP-tasojen seuranta voi auttaa tunnistamaan tulehduksia ja muita siihen liittyviä terveysongelmia.
- Paastoverensokeri: Paastoverenglukoosi on veren glukoosimäärän mitta yön yli paaston jälkeen . Kohonneet verensokeriarvot ovat diabeteksen ja metabolisen oireyhtymän avainindikaattori , jotka liittyvät lisääntyneeseen sydänsairauksien, aivohalvauksen ja muiden kroonisten terveyssairauksien riskiin.
- Hemoglobiini A1C (HbA1C): HbA1C mittaa keskimääräiset verensokeriarvot viimeisen 2–3 kuukauden ajalta. Korkeat HbA1C-tasot osoittavat huonoa glukoositasapainoa ja insuliiniresistenssiä, ja ne on yhdistetty lisääntyneeseen sydänsairauksien, aivohalvauksen ja muiden kroonisten terveyssairauksien riskiin.
- HDL-kolesteroli (HDL): HDL-kolesterolia kutsutaan usein "hyväksi" kolesteroliksi, koska se auttaa poistamaan LDL-kolesterolia tai "pahaa" kolesterolia verenkierrosta. Matala HDL-taso on sydänsairauksien riskitekijä, kun taas korkeat tasot liittyvät pienempään sydänsairauksien ja muiden kroonisten terveyssairauksien riskiin.
- Matalatiheyksinen lipoproteiini (LDL) -kolesteroli: LDL-kolesterolia kutsutaan usein "pahaksi" kolesteroliksi, koska se voi edistää plakin muodostumista valtimoissa. Korkeat LDL-tasot voivat olla sydänsairauksien ja muiden kroonisten sairauksien riskitekijä.
- Triglyseridit: Triglyseridit ovat eräänlainen rasva, joka löytyy verestä. Korkeat triglyseridipitoisuudet on yhdistetty lisääntyneeseen sydänsairauksien, aivohalvauksen ja muiden kroonisten terveyssairauksien riskiin.
- Kokonaiskolesteroli: Kokonaiskolesteroli on HDL-, LDL- ja muiden veren kolesterolihiukkasten summa. Korkeat kokonaiskolesterolitasot ovat sydänsairauksien ja muiden kroonisten terveyssairauksien riskitekijä. Toisaalta alhainen kokonaiskolesteroli voi aiheuttaa D-vitamiinin puutetta, steroidihormonien tuotantoongelmia, masennusta ja lisääntynyttä ennenaikaisen kuoleman riskiä eri syistä .
- Homokysteiini: Homokysteiini on aminohappo, joka voi olla elimistölle myrkyllistä korkeissa määrin. Kohonneet homokysteiinitasot on yhdistetty lisääntyneen oksidatiivisen stressin aiheuttamaan lisääntyneeseen sydänsairauksien ja muiden kroonisten terveyssairauksien riskiin.
- D-vitamiini: D-vitamiini on välttämätön ravintoaine, jolla on ratkaiseva rooli luuston terveydessä, immuunitoiminnassa ja monissa muissa fysiologisissa prosesseissa. Matala D-vitamiinitaso on yhdistetty lisääntyneeseen riskiin sairastua erilaisiin terveysongelmiin, kuten osteoporoosiin, syöpään ja autoimmuunisairauksiin.
- Seerumin rauta: Seerumin rautatasot mittaavat raudan määrää veressä. Rauta on välttämätön ravintoaine, jolla on ratkaiseva rooli punasolujen muodostumisessa. Seerumin korkeat rautatasot on yhdistetty lisääntyneeseen sydänsairauksien ja kuolleisuuden riskiin , kun taas alhaiset tasot voivat johtaa anemiaan.
- Ferritiini: Ferritiini on proteiini, joka varastoi rautaa kehossa. Kohonneet ferritiinitasot osoittavat ylimääräistä raudan varastointia, mikä on yhdistetty lisääntyneeseen riskiin sairastua erilaisiin terveysongelmiin , kuten sydänsairauksiin, syöpään ja diabetekseen. Liian alhainen taso viittaa raudanpuutteeseen.
- Transferriinin saturaatio: Transferriinin saturaatio mittaa transferriiniin sitoutuneen raudan määrää, joka on proteiini, joka kuljettaa rautaa veressä. Kohonneet transferriinin saturaatiotasot voivat viitata liialliseen raudan varastointiin ja lisääntyneeseen riskiin sairastua erilaisiin terveysongelmiin. Liian alhainen taso kertoo raudan puutteesta.
- Täydellinen verenkuva (CBC): CBC mittaa useita veren komponentteja, mukaan lukien punasolut, valkosolut ja verihiutaleet. Se voi auttaa diagnosoimaan ja seuraamaan erilaisia tiloja, kuten anemiaa, infektioita ja leukemiaa.
- Valkosolujen määrä (WBC) : Valkosolujen määrä mittaa veren valkosolujen määrää. Se voi auttaa diagnosoimaan ja seuraamaan infektioita, tulehdusta ja immuunijärjestelmän häiriöitä. Alemmat mutta vertailualueen sisällä olevat tasot liittyvät alentuneeseen kuolleisuusriskiin.
- Punasolujen määrä (RBC): RBC-luku mittaa punasolujen määrää veressä. Se voi auttaa diagnosoimaan ja seuraamaan anemiaa, munuaissairauksia ja luuydinhäiriöitä.
- Hemoglobiini: Hemoglobiini on punasoluissa oleva proteiini, joka kuljettaa happea koko kehossa. Hemoglobiinitesti mittaa veren määrän ja voi auttaa diagnosoimaan ja seuraamaan anemiaa ja muita verisairauksia.
- Hematokriitti: Hematokriitti mittaa punasolujen osuutta veressä. Hematokriittitesti voi auttaa diagnosoimaan ja seuraamaan anemiaa ja kuivumista.
- Keskimääräinen korpuskulaarinen tilavuus (MCV): MCV mittaa punasolujen keskimääräistä kokoa. MCV-testi voi auttaa diagnosoimaan ja seuraamaan anemiaa ja muita verisairauksia.
- Keskimääräinen verisolujen hemoglobiini (MCH): MCH mittaa hemoglobiinin määrän yhdessä punasolussa. MCH-testi voi auttaa diagnosoimaan ja seuraamaan anemiaa ja muita verisairauksia.
- Keskimääräinen verisolujen hemoglobiinipitoisuus (MCHC): MCHC mittaa hemoglobiinipitoisuuden tietyssä punasolujen tilavuudessa. MCHC-testi voi auttaa diagnosoimaan ja seuraamaan anemiaa ja muita verisairauksia.
- Verihiutaleiden määrä: Verihiutaleiden määrä mittaa verihiutaleiden määrää veressä. Se voi auttaa diagnosoimaan ja seuraamaan verenvuotoa, hyytymistä ja luuydinhäiriöitä. Alemmat mutta vertailualueen sisällä olevat tasot liittyvät alentuneeseen kuolleisuusriskiin.
- Fibrinogeeni: Fibrinogeeni on maksassa tuotettu proteiini, joka osallistuu veren hyytymiseen. Veren korkea fibrinogeenitaso voi lisätä sydän- ja verisuonisairauksien ja aivohalvauksen riskiä.
- D-dimeeri: D-dimeeri on proteiinifragmentti, joka syntyy, kun veritulppa hajoaa. Kohonneet D-dimeeritasot veressä voivat viitata verihyytymään tai tromboottiseen häiriöön.
- Eturauhasspesifinen antigeeni (PSA): PSA on miesten eturauhasen tuottama proteiini. Kohonneet PSA-tasot veressä voivat olla merkki eturauhassyövästä tai muista eturauhaseen liittyvistä sairauksista.
- Testosteroni: Testosteroni on kiveksissä tuotettu miessukupuolihormoni. Matala testosteronitaso voi aiheuttaa erilaisia oireita miehillä, mukaan lukien väsymys, libidon heikkeneminen ja lihasheikkous. Lue kattava artikkeli luonnollisesti nostavasta testosteronitasosta täältä.
- Estrogeeni: Estrogeeni on naispuolinen sukupuolihormoni, jota tuotetaan munasarjoissa. Matala estrogeenitaso voi aiheuttaa naisilla erilaisia oireita, kuten kuumia aaltoja, yöhikoilua ja emättimen kuivuutta. Lue lisää estrogeenista ja muista naishormoneista Biohacking Women -verkkokurssilla.
- Follikkelia stimuloiva hormoni (FSH): FSH on aivolisäkkeen tuottama hormoni, joka stimuloi munasarjojen follikkelien kasvua naisilla ja siittiöiden tuotantoa miehillä. Kohonneet FSH-tasot voivat olla merkki vaihdevuosista naisilla tai kivesten vajaatoiminnasta miehillä.
- Luteinisoiva hormoni (LH): LH on aivolisäkkeen tuottama hormoni, joka stimuloi ovulaatiota naisilla ja testosteronin tuotantoa miehillä. Kohonneet LH-tasot voivat olla merkki vaihdevuosista naisilla tai kivesten vajaatoiminnasta miehillä.
- Kilpirauhasta stimuloiva hormoni (TSH): TSH on aivolisäkkeen tuottama hormoni, joka stimuloi kilpirauhasta tuottamaan kilpirauhashormoneja. Kohonnut TSH-taso voi olla merkki kilpirauhasen vajaatoiminnasta tai kilpirauhasen vajaatoiminnasta.
- Vapaa trijodityroniini (fT3): fT3 on yksi kahdesta tärkeimmistä kilpirauhasen tuottamasta kilpirauhashormonista. Matala fT3-taso voi olla merkki kilpirauhasen vajaatoiminnasta tai kilpirauhasen vajaatoiminnasta.
- Vapaa tyroksiini (fT4): fT4 on toinen kilpirauhasen tuottama ensisijainen kilpirauhashormoni. Matala fT4-taso voi olla merkki kilpirauhasen vajaatoiminnasta tai kilpirauhasen vajaatoiminnasta.
- Kilpirauhasen peroksidaasivasta-aine (TPO): Immuunijärjestelmän tuottama vasta-aine voi hyökätä kilpirauhaseen ja aiheuttaa kilpirauhasen vajaatoimintaa. TPO-vasta-aineiden kohonneet tasot voivat olla merkki autoimmuunisairaudesta kilpirauhassairaudesta.
- Adrenokortikotrooppinen hormoni (ACTH): ACTH on aivolisäkkeen tuottama hormoni, joka stimuloi lisämunuaisia tuottamaan kortisolia, steroidihormonia. Kohonneet ACTH-tasot voivat olla merkki lisämunuaisten vajaatoiminnasta tai Cushingin oireyhtymästä.
- Kortisoli: Kortisoli on steroidihormoni, jota lisämunuaiset tuottavat vastauksena stressiin . Se auttaa säätelemään kehon vastetta stressiin ja vaikuttaa verensokerin hallintaan, immuunijärjestelmän toimintaan ja tulehdukseen. Epänormaalit kortisolitasot voivat olla merkki lisämunuaisen toimintahäiriöstä tai muista terveysongelmista.
- Insuliinin kaltainen kasvutekijä 1 (IGF-1): IGF-1 on hormoni, jota maksa tuottaa ensisijaisesti vasteena kasvuhormonille. Se on välttämätöntä normaalille kasvulle ja kehitykselle; epänormaalit tasot voivat liittyä kasvuhäiriöihin ja muihin terveysongelmiin. Sekä matalat että korkeat normaalit IGF-I-tasot liittyvät insuliiniresistenssiin.
- Dehydroepiandrosteroni (DHEA): DHEA on lisämunuaisten tuottama hormoni, jolla on rooli sukupuolihormonien tuotannossa. Epänormaalit DHEA-tasot voivat liittyä lisämunuaisen toimintahäiriöön ja muihin terveysongelmiin.
- Follikulaarisen vaiheen estradioli: Estradioli on eräänlainen estrogeenihormoni, jota munasarjat tuottavat. Kuukautiskierron follikulaarisen vaiheen aikana estradiolitasot nousevat ja sillä on rooli kehon valmistelemisessa ovulaation tapahtumiseen. Epänormaalit estradiolitasot voivat liittyä kuukautishäiriöihin ja muihin terveysongelmiin.
- Luteaalivaiheen progesteroni: Progesteroni on munasarjojen tuottama hormoni, joka on välttämätön kohdun valmistelemiseksi raskauteen. Kuukautiskierron luteaalivaiheessa progesteronitasot nousevat. Epänormaalit progesteronitasot voivat liittyä kuukautishäiriöihin ja muihin terveysongelmiin.
- Kystatiini C: Kystatiini C on kehon solujen tuottama proteiini, jota käytetään munuaisten toiminnan mittaamiseen. Kohonneet kystatiini C:n tasot voivat olla merkki heikentyneestä munuaisten toiminnasta.
- Paastoinsuliini: Paastoinsuliini on verikoe, joka mittaa insuliinin määrää veressä paaston jälkeen. Insuliini on haiman tuottama hormoni, joka auttaa elimistöä säätelemään verensokeritasoja. Korkea paastoinsuliinitaso voi viitata insuliiniresistenssiin tai diabetekseen.
- Kreatiniini: Kreatiniini on jätetuote, jota lihakset tuottavat normaalin aineenvaihdunnan aikana. Se suodattuu verestä munuaisten kautta ja erittyy virtsaan. Verikoetta, joka mittaa veren kreatiniinitason, voidaan käyttää munuaisten toiminnan arvioimiseen. Veren kohonnut kreatiniinitaso voi viitata munuaisten vajaatoimintaan tai vaurioon.
- Virtsahappo: Virtsahappo on jätetuote, joka syntyy, kun keho hajottaa monissa elintarvikkeissa ja kehon soluissa olevia puriineja. Munuaiset erittävät suurimman osan virtsahaposta, mutta jos virtsahappoa muodostuu liikaa tai munuaiset eivät toimi kunnolla, veren virtsahappotasot voivat nousta. Veren korkea virtsahappotaso voi johtaa kihtiin, joka aiheuttaa nivelkipua ja turvotusta. Kohonnut virtsahappopitoisuus voi myös olla ratkaisevampi korjattavissa oleva riskitekijä aineenvaihdunta- ja sydän- ja verisuonisairauksissa.
- Alaniiniaminotransferaasi (ALT): ALT on entsyymi, jota esiintyy pääasiassa maksassa. Se vapautuu verenkiertoon, kun maksasolut ovat vaurioituneet, mikä voi johtua tiloista, kuten hepatiitti, alkoholin väärinkäyttö tai maksasyövä. Kohonneet ALT-arvot veressä voivat viitata maksavaurioon tai -sairauteen. Kohtalaista ALAT-tasojen nousua esiintyy myös aineenvaihduntahäiriöiden, kuten hyperlipidemian, liikalihavuuden ja tyypin 2 diabeteksen yhteydessä.
- Aspartaattiaminotransferaasi (AST): AST on entsyymi, jota esiintyy monissa kehon kudoksissa, mukaan lukien maksa, sydän ja lihakset. Kuten ALT, se vapautuu verenkiertoon solujen vaurioituessa. Kohonneet AST-tasot voivat viitata maksan, sydämen tai lihasten vaurioitumiseen.
- Gamma-glutamyylitransferaasi (GGT): GGT on maksassa, haimassa ja muissa elimissä esiintyvä entsyymi. Se osallistuu glutationin, antioksidantin, aineenvaihduntaan, joka auttaa suojaamaan soluja vaurioilta. Kohonneet GGT-tasot veressä voivat viitata maksa- tai sappitiesairauksiin ja liialliseen alkoholinkäyttöön.
Suurin osa näistä merkeistä (95 %) on käsitelty erittäin yksityiskohtaisesti suosituimmassa terveyden optimoinnin oppimisalustassamme; Optimoi laboratoriotulokset -verkkokurssi!
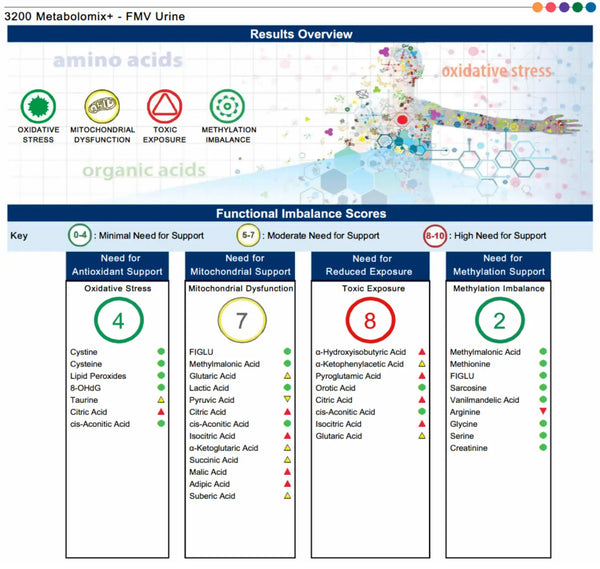
Orgaanisten happojen testi (OAT)
Organic Acids Test (OAT) on diagnostinen työkalu, joka mittaa orgaanisten happojen metaboliitteja virtsassa. Näitä aineenvaihduntatuotteita elimistö tuottaa erilaisten aineenvaihduntareittien seurauksena, ja ne voivat antaa tietoa ravinteiden puutteesta, energiantuotannosta ja suoliston mikrobiomin terveydestä.
OAT voi havaita ja seurata erilaisia tiloja, mukaan lukien ravinteiden puutteita, tulehdusta, oksidatiivista stressiä, mitokondrioiden toimintahäiriöitä ja poikkeavuuksia välittäjäaineiden aineenvaihdunnassa. Se voi myös tunnistaa haitallisten bakteerien tai hiivan liikakasvun suolistossa ja epätasapainoa suoliston mikrobiomissa, mikä voi vaikuttaa moniin terveysongelmiin.
Yksi OAT:n tärkeimmistä eduista on, että se voi tarjota kattavan kuvan yksilön aineenvaihduntaprofiilista , mukaan lukien tietoa siitä, kuinka hänen kehonsa käsittelee erilaisia ravintoaineita ja kuinka hyvin heidän mitokondrionsa toimivat. OAT voi auttaa terveydenhuollon ammattilaisia räätälöimään ravitsemus- ja lisätoimenpiteitä yksilön yksilöllisten tarpeiden mukaan tunnistamalla ravintoaineiden puutteet ja epätasapainot. Lisäksi tunnistamalla suoliston mikrobiomin epätasapainoa OAT voi auttaa ohjaamaan ruokavalio- ja elämäntapatoimenpiteitä, jotka voivat parantaa suoliston terveyttä ja yleisiä terveysvaikutuksia.
Suosittelemme Metabolomix+ -kotitestin tekemistä.
Metabolomixin aineenvaihdunta-alueet + analyysi:
Perusprofiili:
- Orgaaniset hapot
- Imeytymishäiriöt ja dysbioosi
- Soluenergia ja mitokondriot
- Sovittelijat
- Vitamiinimerkkiaineet
- Toksiini- ja vieroitusmerkit
- Tyrosiinin aineenvaihdunta
- Aminohapot
- Välttämättömiä aminohappoja
- Ei-välttämättömät aminohapot
- Aineenvaihdunnan välituotteet
- Markkerit ravinnon peptideille
- Oksidatiivisen stressin merkkiaineet
Katso täydellinen Metabolomix+ -näyteraportti täältä.
Aminohapot (virtsa)
Aminohapot sisältävät neljä olennaista alkuainetta: hiiltä (C), vetyä (H), happea (O) ja typpeä (N). Ihmiselle tärkeitä aminohappoja on kaksikymmentä, joista yhdeksän on välttämättömiä (täytyy saada ravinnosta), ja loput yksitoista syntetisoituvat elimistössä. Siten aminohapot luokitellaan välttämättömiin ja ei-välttämättömiin aminohappoihin. Osa välttämättömistä aminohapoista luokitellaan edelleen ehdollisesti välttämättömiksi tai ehdollisesti välttämättömiksi, eli ne on saatava ravinnosta, koska niiden syntetisoitu määrä ei pysty täysin vastaamaan elimistön tarpeita.
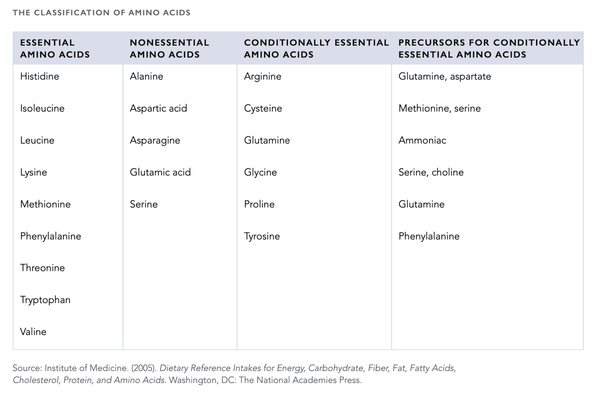
Keho tarvitsee aminohapoista muodostuvia proteiineja useiden eri tehtävien hoitamiseen. Ne ovat seuraavat:
- Kudosten kasvu ja uusiutuminen
- Vaurioituneen kudoksen korjaaminen
- Detoksifikaatio
- Ruoansulatus (ruoansulatusentsyymit)
- Entsyymit ja kofaktorit (ne katalysoivat kemiallisia reaktioita kehossa)
- Rakenteelliset komponentit (kudoksissa ja solukalvoissa)
- Kemiallisten prosessien (koentsyymit jne.) nopeuttaminen ja säätely
- Toimii biologisina siirtoproteiineina (esim. hemoglobiini)
- Immuunijärjestelmän toiminnan ylläpitäminen (vasta-aineet ja immunoglobuliinit)
- Välittäjät ja signaalin välittäjät
- Toimii hormonina
- Ferritiinin varastointi
- Energian tuotanto
- Solujen liike
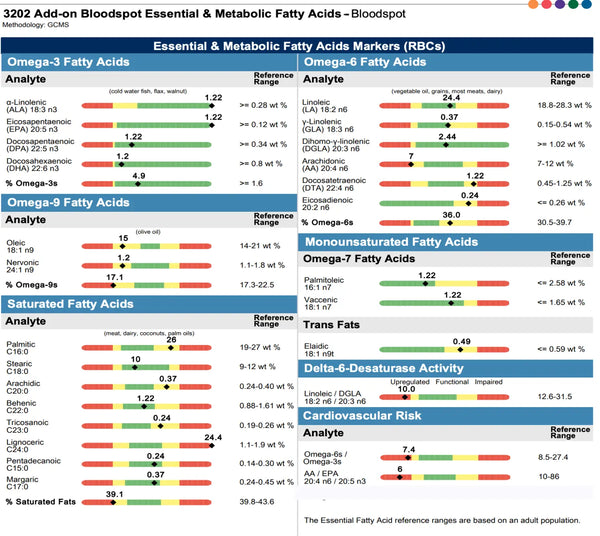
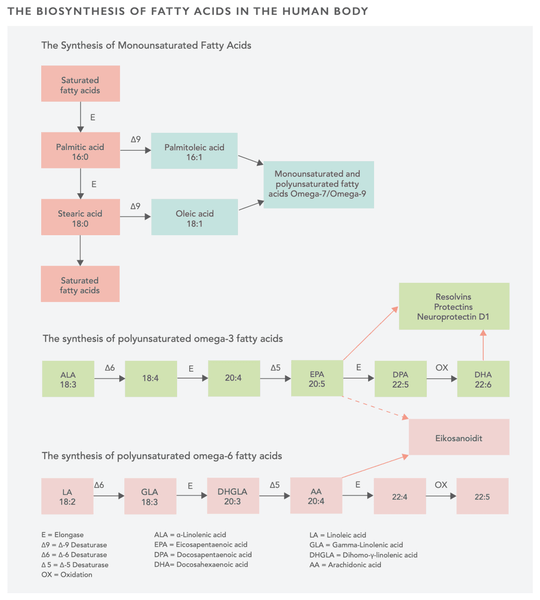
Rasvahapot (veri)
Rasvahapot ovat kemiallisia yhdisteitä, jotka koostuvat hiilestä, vedystä ja karboksyyliryhmästä, joka sisältää myös happea. Rasvahapot ovat monokarboksyylihappoja, joissa on aina tasainen määrä hiiliatomeja. Luonnossa ne muodostavat eripituisia hiiliketjuja, jotka määrittävät rasvahappojen luokan (lyhytketjuiset rasvahapot, keskipitkäketjuiset rasvahapot, pitkäketjuiset rasvahapot ja erittäin pitkäketjuiset rasvahapot).
Keho voi syntetisoida lyhytketjuisia rasvahappoja suolistossa suolistobakteerien avulla. Lisäksi keskipitkäketjuisia rasvahappoja löytyy myös luonnosta (esim. kookospähkinästä). Rasvahappojen kyllästysaste riippuu mahdollisista kaksoissidoksista hiiliketjujen välillä. Tyydyttyneet rasvahapot sisältävät vain yksittäisiä sidoksia. Kertatyydyttymättömissä rasvahapoissa on yksi kaksoissidos hiiliatomien välillä ja monityydyttymättömissä rasvahapoissa useita sidoksia. Näin ollen rasvahapot voivat olla joko tyydyttyneitä, kertatyydyttymättömiä tai monityydyttymättömiä.
Rasvahapot vaikuttavat solujen signalointiin kehossa ja muuttavat geenien ilmentymistä rasva- ja hiilihydraattiaineenvaihdunnassa. Lisäksi rasvahapot voivat toimia ligandeina peroksisomin proliferaatio-aktivoimille reseptoreille (PPAR), joilla on olennainen rooli muun muassa tulehduksen (eli eikosanoidien), rasvanmuodostuksen (adipogeneesi), insuliinin ja neurologisten toimintojen säätelyssä.
Rasvahappojen lisäosa Metabolomix+:lle
Tämä lisäosa voidaan lisätä Metabolomix+ -testiin, ja se kattaa välttämättömät ja metaboliset rasvahapot helposti kotona tehtävällä veripistesormenpistolla.
Tämän lisäosan kattamat analyytit:
- Omega 3 rasvahapot ovat välttämättömiä aivojen toiminnalle ja sydän- ja verisuoniterveydelle ja ovat tulehdusta estäviä
- Omega 6 rasvahapot ovat mukana tulehduksen tasapainottamisessa
- Omega 9 rasvahapot ovat välttämättömiä aivojen kasvulle, hermosolujen myeliinille ja tulehduksen vähentämiselle
- Tyydyttyneet rasvahapot osallistuvat lipoproteiinien aineenvaihduntaan ja rasvakudostulehdukseen
- Monityydyttymättömät rasvat sisältää omega-7-rasvoja ja epäterveellisiä transrasvoja
- Delta-6 Desaturase Activity arvioi tämän entsyymin tehokkuuden omega 6:n ja omega 3:n metaboloinnissa
- Kardiovaskulaarinen riski sisältää tietyt suhteet ja Omega-3-indeksin
Suolen mikrobiomi ja mikrobiota – keskeinen testi kaikille
Mikrobiomi ja mikrobiota ovat joskus vaihdettavissa keskenään, mutta nämä termit eroavat toisistaan. Mikrobiomi on genomien kokoelma kaikista ympäristössä olevista mikro-organismeista. Esimerkiksi ihmisen mikrobiomi viittaa mikro-organismien ryhmään kehon ympärillä (mukaan lukien iho, silmät, suolisto ja niin edelleen). Mikrobiota viittaa yleensä tiettyihin mikro-organismeihin, joita löytyy tietystä ympäristöstä. Tässä tapauksessa mikrobiota (eli suoliston mikrobiota) viittaa kaikkiin suolistossa esiintyviin mikro-organismeihin, kuten bakteereihin, viruksiin ja sieniin.
Arvioiden mukaan suolistossa elää 500–1 000 erilaista bakteerilajia. Suolistossa yleisimmät bakteerilajit ovat Bacteroides, Clostridium, Fusobacterium ja Bifidobacterium. Muita tunnettuja kantoja ovat Escherichia ja Lactobacillus. Bifidobacterium- ja Lactobacillus- kannat ovat tyypillisesti läsnä probioottivalmisteissa, koska ne ovat laajimmin tutkittuja.
Suolistossa olevien bakteerien tehtäviin kuuluu hiilihydraattien hajottaminen (käyminen), joita elimistö ei muuten pysty sulattamaan. Suoliston bakteerikannat osallistuvat myös K-vitamiinien, B-vitamiinien ja joidenkin kivennäisaineiden (magnesiumin, kalsiumin ja raudan) imeytymiseen sappihappojen tuotannossa ja immuunijärjestelmässä. Lisäksi ne toimivat suojaseininä erilaisia taudinaiheuttajia vastaan.
Suolen bakteerikanta muuttuu nopeasti aina, kun ruokavaliota muutetaan. Hiirillä tehdyt tutkimukset ovat osoittaneet, että mikrobiota voi muuttua yön aikana ruokavaliota muuttaessa. Samanlaisia muutoksia tapahtuu myös ihmisillä, mutta tarkkaa ajanjaksoa ei tunneta. Suolistoystävällisempään ruokavalioon siirtyminen on tuonut myönteisiä tuloksia kroonisen tulehduksen, liikalihavuuden ja suoliston läpäisevyyden hoidossa .
GI360 – Suolistotestien Lamborghini
Henkilökohtainen hoitostrategia on lääketieteen tulevaisuus. Se perustuu yksilölliseen biokemiaan ja geneettiseen perintöön liittyviin tietoihin. Tämä testi auttaa sinua saamaan objektiivista tietoa itsestäsi, luomaan tarkemman hoitostrategian ja toteuttamaan muutoksia, jotka johtavat parempaan terveyteen.
Suoliston GI360 x3 -määritys käyttää useita seulontamenetelmiä (multipleksi-PCR, MALDI-TOF ja mikroskopia) patogeenien, virusten, loisten ja bakteerien havaitsemiseen. Nämä voivat ilmetä akuuteina tai kroonisina maha-suolikanavan oireina ja sairauksina tai mahdollisesti suolistoon liittyvinä oireina.
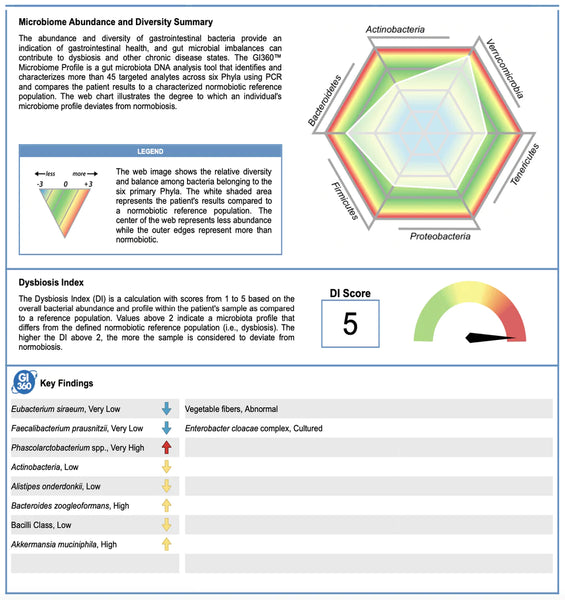
Kuva: Esimerkkiraportin ensimmäisen sivun analyysi GI 360 -testistä.
Mikrobiomin runsaus ja monimuotoisuus
GI360™ Profile on suoliston mikrobiotan DNA-analyysityökalu, joka tunnistaa ja luonnehtii yli 45 kohdennetun analyytin runsautta ja monimuotoisuutta, joiden vertaisarvioitu tutkimus on osoittanut edistävän dysbioosia ja muita kroonisia sairaustiloja.
Dysbioosiindeksi (DI) on laskelma, jonka arvot ovat 1–5, jotka perustuvat potilaan näytteen bakteerien yleiseen määrään ja profiiliin verrattuna vertailupopulaatioon. Arvot yli 2 osoittavat mikrobiotaprofiilin, joka eroaa määritellystä normobioottisesta vertailupopulaatiosta (eli dysbioosista). Mitä korkeampi DI on yli 2, sitä enemmän näytteen katsotaan poikkeavan normobioosista.
Näitä tietoja voidaan käyttää muun muassa yksilöllisen hoitoohjelman harkitsemiseen ja rakentamiseen.
Testi soveltuu erityisen hyvin käytettäväksi seuraavissa suolistosairauksissa ja kroonisissa ongelmissa:
- Ruoansulatuskanavan oireet
- Autoimmuunisairaudet
- IBD / IBS
- Tulehdukset
- Ruoka-aineyliherkkyys
- Ravitsemukselliset puutteet
- Nivelkipu
- Krooninen tai akuutti ripuli
- Veriset ulosteet
- Limakalvojen toimintahäiriö
- Vatsakipu
- Kuume ja oksentelu
Laaja GI360 x3 suolianalyysi on tällä hetkellä tarkin ja kattavin analyysi ruoansulatuskanavan kokonaistasapainosta. Myös monet funktionaalisen lääketieteen lääkärit ympäri maailmaa käyttävät testiä.
Geneettinen testaus (DNA) ja sen valtavat mahdollisuudet
Geneettisen koodisi tuntemisen mahdollistavat uudet DNA-testit, jotka perustuvat uusimpaan tieteeseen ja teknologiaan. Ne voivat auttaa tekemään parempia valintoja jokapäiväisessä elämässä ja löytämään tehokkaampia tapoja muuttaa elämäntapoja. Samalla DNA-testit auttavat optimoimaan terveyttä ja saavuttamaan henkilökohtaisia tavoitteita.
Geenitestaus on tehokas työkalu, joka on mullistanut terveydenhuollon alan. Sen avulla yksilöt voivat saada käsityksen geneettisestä rakenteestaan ja ymmärtää paremmin riskiään sairastua tiettyihin sairauksiin tai tiloihin. Analysoimalla yksilön DNA :ta geneettinen testaus voi paljastaa tietoa geneettisistä mutaatioista, muunnelmista ja muutoksista, jotka voivat vaikuttaa merkittävästi yksilön terveyteen. Näiden tietojen avulla yksilöt voivat tehdä tietoisempia päätöksiä terveydestään, mukaan lukien elämäntapamuutokset ja ennaltaehkäisevät toimenpiteet, vähentääkseen riskiään sairastua tiettyihin sairauksiin.
Lisäksi geneettisellä testauksella voidaan diagnosoida ja hoitaa erilaisia sairauksia ja tarjota yksilöllisiä ja kohdennettuja hoitoja, jotka voivat parantaa merkittävästi potilaiden tuloksia. Geenitestauksen merkitystä terveydenhuollossa ei voi liioitella, ja tekniikan kehittyessä se voi mahdollisesti muuttaa tapaamme lähestyä sairauksien ehkäisyä ja hoitoa.
I ntegraal DNA: Kolmen DNA-testin yhdistelmä (resilienssi + terveys + aktiivisuus)
Tarkkuusravitsemus, tarkkuuslääketiede ja nutrigenomiikka ovat kaikki toisiinsa liittyviä käsitteitä, jotka mullistavat ajattelumme terveydestä ja ravitsemuksesta. Pohjimmiltaan nämä termit viittaavat kehittyneen teknologian ja datan käyttöön henkilökohtaisten terveyssuunnitelmien luomiseen . Yksilön DNA:n ja elämäntavan ymmärtäminen voi räätälöidä nämä suunnitelmat vastaamaan henkilön ainutlaatuisia tarpeita.
Integral DNA:n avulla saat kolme tehokasta uutta geneettistä testiä, jotka auttavat sinua tekemään parempia elämänvalintoja ja tehokkaampia elämäntapamuutoksia. Kun tiedät geneettisen koodisi, voit avata kehosi salaisuudet optimoidaksesi terveyden ja saavuttaaksesi henkilökohtaiset tavoitteesi.
Testisarja koostuu kolmesta eri geneettisestä testistä, jotka antavat sinulle kattavan kuvan terveydestäsi. Aikaisemmin yhden geenitestin hinnalla saat kolme.
DNA Terveys
DNA Health® testaa tunnettuja geneettisiä muunnelmia, jotka vaikuttavat merkittävästi terveyteen ja erilaisiin sairauksien, kuten osteoporoosin, syövän, sydän- ja verisuonitautien ja diabeteksen riskeihin.
DNA aktiivinen
DNA Active analysoi geenejä, joiden on havaittu vaikuttavan merkittävästi seuraaviin alueisiin: pehmytkudosvaurioriski, palautuminen, voimantuotantopotentiaali, kestävyyspotentiaali, kofeiiniaineenvaihdunta, suolaherkkyys ja huippusuorituksen ajoitus.
DNA-resilienssi
DNA Resilience tarjoaa tietoa seitsemästä keskeisestä molekyylialueesta, jotka vaikuttavat stressiin ja kestävyyteen eniten. Näitä ovat neuropeptidi Y, oksitosiini, neurotrofiset tekijät, kortisoli, norepinefriini, dopamiini ja serotoniini.
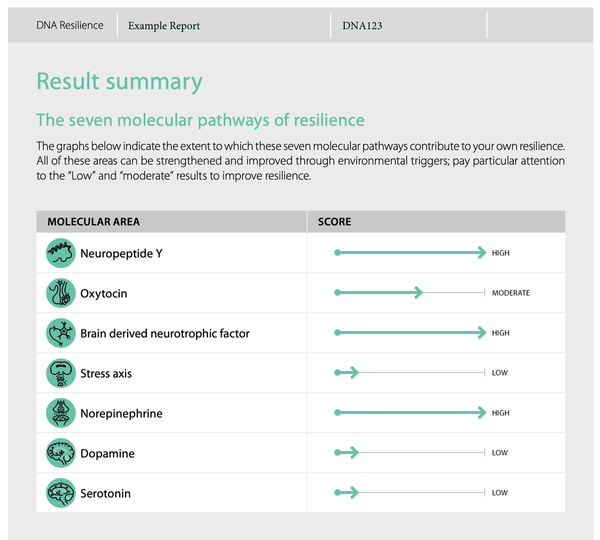
Kuva : Esimerkki yhteenveto DNA Resilience -testistä.
Lue lisää Integral DNA -testistä täältä.
Epigeneettinen testaus – ehkäisevän lääketieteen tulevaisuus?
Epigenetiikka tutkii, kuinka geeniekspression muutoksia voi tapahtua ilman muutoksia taustalla olevassa DNA-sekvenssissä. Useat tekijät, kuten ympäristöaltistuminen, elämäntapavalinnat ja muut ulkoiset vaikutukset, voivat vaikuttaa tähän.
Ihmisen terveyden kannalta epigenetiikan uskotaan vaikuttavan erilaisiin tiloihin, mukaan lukien syöpä, sydän- ja verisuonitaudit ja neurologiset sairaudet. Ymmärtämällä paremmin epigeneettisten muutosten taustalla olevia mekanismeja tutkijat toivovat voivansa kehittää uusia hoitoja ja interventioita, jotka voivat ehkäistä tai hoitaa näitä tiloja.
Jotkut tekijät, joiden on osoitettu vaikuttavan epigeneettisiin muutoksiin, ovat ruokavalio, liikunta, stressi ja altistuminen myrkkyille ja saasteille. Geneettisillä tekijöillä voi myös olla rooli yksilön alttiuden määrittämisessä epigeneettisille muutoksille.
Vaikka genetiikan, epigenetiikan ja ympäristötekijöiden monimutkaisesta vuorovaikutuksesta ei vielä tiedetä paljon, tämän alan tutkimus edistyy nopeasti. Se voi mullistaa ymmärryksemme ihmisten terveydestä ja sairauksista.
Epigenomi on dynaaminen järjestelmä, jolla on merkittävä rooli ikääntymisessä. DNA:n metylaatio ja histonimuunnelmat muuttuvat kronologisen iän ja kroonisten sairauksien mukaan. Ikääntyminen liittyy yleiseen hypometylaatioon ja paikalliseen hypermetylaatioon. DNA-metylaation analysoimiseksi asianmukaisesti on kehitetty erilaisia "epigeneettisiä kelloja" ( kuten Horvath-kello, Weidner-kello ja Hannum-kello ).
Epigeneettisten modifikaatioiden tyypit
Useita erilaisia epigeneettisiä modifikaatioita voidaan mitata, joista jokainen voi tarjota tärkeitä näkemyksiä yksilön terveydestä ja sairausriskistä. Näitä ovat:
- DNA:n metylaatio: Tämä lisää metyyliryhmän tiettyyn kohtaan DNA-molekyylissä, mikä voi muuttaa geenien ilmentymistä. Epänormaalit metylaatiomallit on liitetty useisiin sairauksiin, mukaan lukien syöpä ja sydän- ja verisuonitaudit.
- Histonimuunnos: Histonit ovat proteiineja, jotka auttavat pakata DNA:ta tiiviiksi rakenteeksi. Histonien modifiointi voi muuttaa geenien saavutettavuutta joko edistämällä tai estämällä niiden ilmentymistä.
- Koodaamaton RNA: Koodaamattomat RNA-molekyylit eivät koodaa proteiineja, mutta voivat säädellä geenin ilmentymistä olemalla vuorovaikutuksessa muiden RNA-molekyylien tai proteiinien kanssa.
- Kromatiinin rakenne: Tapa, jolla DNA pakataan kromatiiniin, voi myös vaikuttaa geenien ilmentymiseen, ja kromatiinin rakenteen muutokset on yhdistetty erilaisiin sairauksiin.
Ikääntyminen on erittäin monimutkainen ja erittäin yksilöllinen prosessi, joka on ymmärrettävä täysin. Siksi monet ikääntymiseen liittyvät biomarkkerit voivat vain naarmuttaa pintaa ja antaa tietyn näkökulman ikääntymiseen liittyviin asioihin. Näin ollen laaja-alaisten rutiinilaboratoriotestien, epigeneettisten testien, molekyylibiomarkkerien ja fenotyyppisten markkerien yhdistelmä voi olla paras ratkaisu arvioida kokonaisvaltaista näkemystä yksittäisestä ikääntymisprosessista.
Biohacker Center tarjoaa tulevaisuuden huippuluokan epigeneettiset testit.
Toistaiseksi suosittelemme GlycanAge-testin suorittamista, joka on kotona tehtävä verikoe, joka analysoi elimistössä olevia glykaaneja (soluja päällystäviä sokereita) biologisen ikäsi määrittämiseksi. He tarkastelevat IgG-glykoomikoostumustasi (joka säätelee matala-asteista kroonista tulehdusta ja ajaa ikääntymistä). GlycanAge-teknologia ylittää olemassa olevat biologiset ikätestit integroimalla ikääntymisen geneettiset, epigeneettiset ja ympäristölliset näkökohdat.
Ennaltaehkäisevä terveys korostuu entisestään ja halu personoida ja validoida terveydenhuoltotoimenpiteitä. GlycanAge on järkevin paikka seurata elämäntapamuutoksia, koska se tarjoaa itsenäisen terveyden mittarin.
Lue lisää GlycanAge-testistä täältä.
Johtopäätös
Täydellisen yleisen terveydentilan arvioimiseksi on erittäin suositeltavaa käyttää tässä artikkelissa mainittuja biomarkkereita ja luottaa nykyiseen tieteelliseen tietoon ihmisen fysiologiasta. On suositeltavaa suorittaa kaikki nämä testit vähintään kerran ja seurata testiä elintapojen muutosten jälkeen 6–12 kuukauden kuluttua arvioidaksesi niiden vaikutusta fysiologiaasi, biokemiaasi ja epigenetiikkaasi.
Saadaksesi kokonaisvaltaisen näkemyksen terveydestäsi, suosittelemme, että käyt läpi kattavan veren biomarkkeripaneelin, orgaanisten happojen testin, aminohapot (jotka sisältyvät orgaanisten happojen testiin), rasvahapot (orgaanisten happojen testin lisänä), kattava mikrobiotesti, integraalinen DNA-testi ja epigeneettinen testi. Nämä testit on suunniteltu antamaan sinulle tarkempi ja syvällisempi käsitys terveydestäsi. Seurantatestillä elämäntapamuutosten tekemisen jälkeen voit seurata edistymistäsi ja tehdä tietoisempia päätöksiä terveydestäsi.