The study of resilience through the lens of genetics is an expanding field of interest, often intersecting with the disciplines of psychology, neurobiology, and genomics. While the concept of resilience – the ability to recover from or adapt to adversity or stress – is multifaceted and influenced by a complex interplay of genetic, environmental, and psychological factors, specific DNA tests have been developed to shed light on the genetic components of this trait.
Introduction
Genes are segments of DNA that contain the instructions the body needs to make each of the many thousands of proteins required for life. Each gene comprises thousands of combinations of "letters" (called bases) that make up your genetic code. The code gives the instructions to make the proteins required for proper development and function.(1)
Genetic variations can affect the expression of a gene, thereby affecting metabolic processes that are important for maintaining cellular health and how we respond to environmental interventions such as diet, lifestyle, supplements and medication.
Knowledge of these genetic variations offers unparalleled insight into biological systems, allowing healthcare practitioners to recommend precise interventions aimed at helping to reach one's goals and achieve optimal health.
Understanding Genetic Markers of Resilience
Resilience—the ability to recover from or adjust easily to adversity or change—is increasingly seen through genetics. By examining genetic markers, researchers and clinicians aim to uncover the biological underpinnings that could explain why some individuals bounce back from stress and trauma more effectively than others.(2) This burgeoning field of investigation has focused on resilience-related DNA tests that examine genetic markers potentially responsible for the differences in individual stress responses.
At the heart of this research lies the endocrine and nervous systems (the autonomic nervous system, in particular) central to the body's response to stress. The hypothalamic-pituitary-adrenal (HPA) axis, in particular, is a central focus area as it plays a critical role in regulating the body's stress response mechanism. This complex network of interactions between the hypothalamus, the pituitary gland and the adrenal glands orchestrates the production and regulation of key stress hormones, such as cortisol.
Cortisol has far-reaching effects on many bodily functions and is released in response to stress and low blood-glucose concentration. Under normal circumstances, cortisol helps restore homeostasis after stressful events. However, gene variations that affect the HPA axis can lead to differences in how cortisol is produced, regulated and cleared from the body. These genetic variations can influence an individual's physiological resilience — their ability to maintain or quickly return to psychological and physical health after hardship.(3)
DNA tests for resilience investigate gene variants associated with the receptors for stress hormones, proteins involved in the stress hormone pathways and enzymes that metabolize these hormones. For example, a variant of the FKBP5 gene, which is involved in regulating the sensitivity of the glucocorticoid receptor through which cortisol exerts its effects, could modify an individual's stress response and potentially their susceptibility to stress-related disorders. Further expanding the scope, genes that encode for neurotransmitters – the brain's chemical messengers that contribute to mood regulation and cognition – are also under the spotlight. These include genes like COMT, which is instrumental in the breakdown of dopamine, a neurotransmitter associated with pleasure and reward systems.(4)
Additionally, inflammation is a biological process that has been closely linked with stress and mood disorders. Chronic inflammation, which genetic variations can influence, can affect brain function and behavior.(5) Thus, genetic tests may also seek to identify variants in pro-inflammatory cytokine genes, such as IL-6 and TNF, which could predispose individuals to prolonged inflammatory responses and affect their mental resilience.
Understanding these genetic markers is the cornerstone for personalized interventions. By identifying genetic predispositions, individuals can take proactive steps to bolster their resilience through lifestyle modifications, psychological strategies, and medical treatments tailored to their unique genetic makeup. This approach exemplifies the shift toward precision medicine, where the one-size-fits-all model gives way to more individualized care.
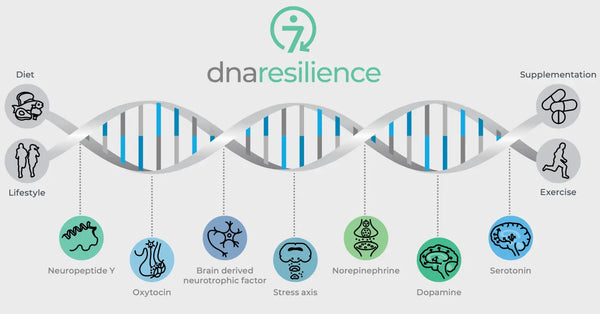
Image: The seven molecular pathways of resilience.
Types of DNA Tests for Resilience
1) Stress Response Genes
Stress response genes are critical components of our body's system for managing and responding to stressors. They encode proteins that regulate various physiological processes, including the release and action of cortisol, a hormone pivotal in the stress response.
CRHR1 (Corticotropin-Releasing Hormone Receptor 1)
CRHR1 encodes a receptor for corticotropin-releasing hormone (CRH), a central hormone initiating the stress response. When CRH binds to CRHR1, it stimulates the production and release of adrenocorticotropic hormone (ACTH), which prompts the adrenal glands to produce cortisol. Variants in the CRHR1 gene can influence how sensitive this receptor is to CRH, which can alter the overall stress response. For instance, some polymorphisms might lead to a heightened stress response, which could contribute to anxiety or depression. In contrast, others may dampen the response, impacting the ability to handle acute stress.(6-7)
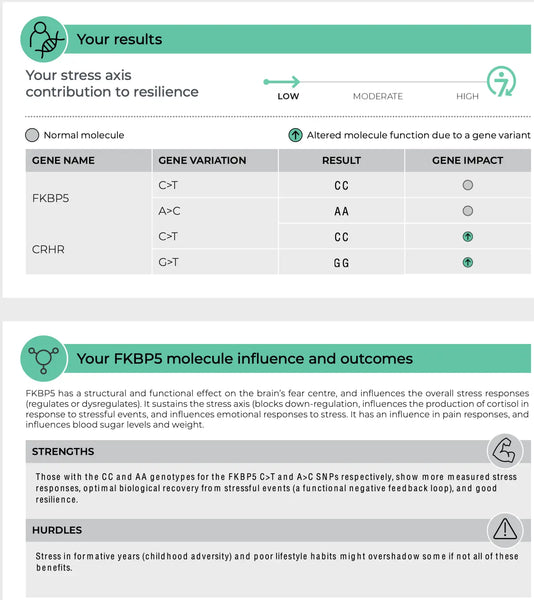
FKBP5 (FK506 Binding Protein 5)
The FKBP5 gene plays a role in regulating the sensitivity of the glucocorticoid receptor, which is the receptor through which cortisol exerts its effects. Specific polymorphisms in FKBP5 have been linked to altered feedback inhibition of the HPA axis and differential responses to glucocorticoids. For example, some variants of FKBP5 can reduce the affinity of the glucocorticoid receptor for cortisol, potentially leading to an impaired stress response and an increased risk for stress-related psychiatric disorders like PTSD or major depression.(8-9)
Image: An example page of the DNA Resilience test.
NR3C1 (Nuclear Receptor Subfamily 3, Group C, Member 1)
NR3C1 encodes the glucocorticoid receptor itself. Variations in this gene can affect how the body reacts to cortisol. Specific polymorphisms in NR3C1 may influence the sensitivity or density of glucocorticoid receptors, affecting how effectively cortisol can carry out its functions. This can lead to a range of responses, from a muted stress response that may hinder an individual from reacting adequately to stressors to an exaggerated response that might result in chronic stress symptoms and even depression.(10-12)
The results from stress response gene testing can give insights into an individual's predisposition to stress-related health issues. For example:
-
Heightened Stress Response: Individuals with specific variants might be more reactive to stress and experience higher cortisol levels during stressful events.
-
Reduced Stress Response: Conversely, some individuals might have a blunted stress response, which could be protective in acute stress situations but might also hinder the activation of necessary physiological mechanisms in response to challenges.
2) Neurotransmitter Function Tests Explained
Neurotransmitter function tests are designed to investigate the genetic factors that influence how neurotransmitters are synthesized, released and broken down in the brain. Since neurotransmitters are chemical messengers that regulate mood, cognition and stress responses, variations in genes related to these substances can have significant implications for an individual's psychological resilience and overall mental health.
Exploring neurotransmitter function in the context of resilience and stress response extends beyond just the catecholamines like dopamine. It includes a broader spectrum of neurotransmitter systems involved in mood regulation, alertness and cognitive function. Several genes are involved in the synthesis, signaling and breakdown of these neurotransmitters, including dopamine beta-hydroxylase (DBH), dopamine receptors (DRD2, DRD4) and various serotonin-related genes.(13)
COMT (Catechol-O-Methyltransferase)
The COMT gene is one of the most extensively studied concerning neurotransmitter function. It encodes an enzyme that breaks down catecholamines—such as dopamine, epinephrine, and norepinephrine—neurotransmitters critical for stress response, cognition, and emotion regulation.
There are well-known polymorphisms in the COMT gene, such as the Val158Met variant. This variant can affect the enzyme's activity level in different ways:(14-15)
- High-activity form (Val variant): This form of the enzyme breaks down dopamine at a faster rate, which can lead to lower levels of dopamine in the prefrontal cortex, a brain region involved in executive function and decision-making. Individuals with this variant may perform better in tasks under stable conditions but might be more susceptible to cognitive decline under stress due to lower dopamine availability.
- Low-activity form (Met variant): Conversely, this form of the COMT enzyme metabolizes dopamine more slowly, resulting in higher dopamine levels in the brain. This can enhance cognitive function under stress but may also increase the risk of stress-related psychopathologies, like anxiety disorders, as the brain is potentially overstimulated by excess dopamine.
Dopamine Beta-Hydroxylase (DBH)
DBH is an enzyme that converts dopamine into norepinephrine, a neurotransmitter involved in the fight-or-flight response. Genetic variations in the DBH gene can affect enzyme activity, influencing dopamine and norepinephrine levels in the brain and peripheral nervous system.(16-18)
- Low Activity: Variants associated with lower DBH activity can lead to higher levels of dopamine and reduced levels of norepinephrine, which may affect cognitive functions such as attention and decision-making and influence how an individual responds to stress.
- High Activity: Conversely, variants that result in higher DBH activity can lower dopamine levels while increasing norepinephrine, potentially impacting stress reactivity and anxiety.
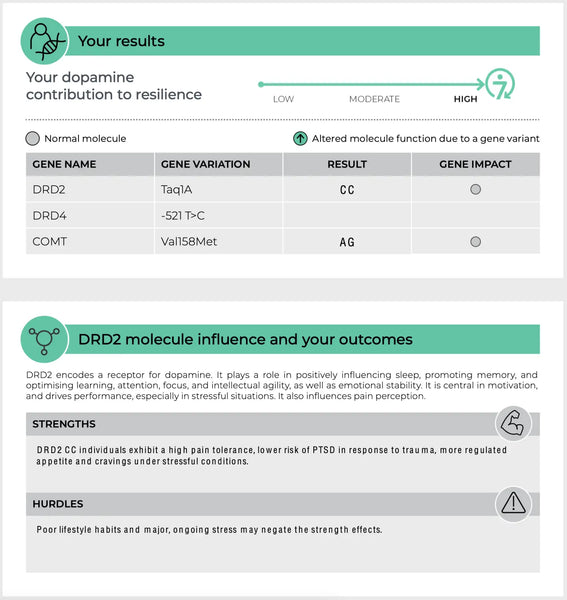
Dopamine Receptors (DRD2 and DRD4)
DRD2 and DRD4 are genes that encode dopamine receptors D2 and D4, respectively. These receptors are part of the dopamine system that regulates numerous functions, including mood, reward, and motor control.(19-20)
- DRD2: Variants in the DRD2 gene can impact the density and binding affinity of D2 receptors. This may influence vulnerability to stress and the efficacy of reward-related cues, with potential implications for conditions such as addiction and depression.
- DRD4: The DRD4 gene is known for a variable number of tandem repeats (VNTR) in the coding region. Specific repeats are associated with traits like novelty seeking and the risk for attention disorders. This polymorphism can affect the efficiency of synaptic dopamine signaling and has been studied in the context of behavioral and psychological resilience.
Image: An example page of the DNA Resilience test.
Serotonin Gene Variations
Serotonin is another crucial neurotransmitter in the regulation of mood, appetite, and sleep, all of which can be affected by stress. Several genes involved in serotonin signaling are of interest:
- 5-HTT (SLC6A4): This gene encodes the serotonin transporter, responsible for serotonin reuptake from the synaptic cleft. The 5-HTTLPR polymorphism in the promoter region of this gene has been studied for its association with stress sensitivity and mood disorders.(21)
- MAOA: The monoamine oxidase A gene is responsible for breaking down serotonin. Variations in this gene can affect serotonin levels and have been associated with behavioral traits and susceptibility to stress.(22)
- TPH2: Tryptophan hydroxylase-2 is an enzyme critical for synthesizing serotonin in the brain. Genetic variations in TPH2 can influence serotonin production, potentially impacting emotional regulation and response to stress.(23)
The interpretation of results from these tests can be complex. For example, a variant associated with a higher risk for stress-related conditions does not necessarily mean an individual will develop such conditions, but it may suggest an increased vulnerability. Similarly, possessing a "resilience" variant does not guarantee an unassailable resistance to stress, as environmental factors and lifestyle choices play substantial roles.
3) Inflammation and its Impact on the brain
Chronic inflammation can be detrimental to brain health. It is thought to contribute to the development and progression of neurodegenerative diseases and may influence the brain's stress response, which is closely tied to resilience. Pro-inflammatory cytokines, like interleukin-6 (IL-6) and tumor necrosis factor (TNF), can cross the blood-brain barrier and interact with the pathways that regulate mood, motivation, and alertness.(24)
Gene Variants Associated with Inflammation
IL-6 (Interleukin-6)
IL-6 is a cytokine that plays a role in the inflammatory response and is involved in various biological functions, including the immune response, hematopoiesis, and bone metabolism. In the context of stress and resilience IL-6 is related to the following:(25-26)
- Elevated IL-6 levels have been associated with a greater risk of developing depression and other mood disorders.
- Specific genetic variants of the IL-6 gene can lead to increased expression of IL-6, potentially exacerbating the inflammatory response and altering the brain's ability to cope with stress.
TNF (Tumor Necrosis Factor)
TNF is another cytokine involved in systemic inflammation. It has various roles, including regulating immune cells and the induction of fever, apoptosis, and inflammation.(27)
- Overexpression of TNF has been linked to various chronic diseases, including rheumatoid arthritis, inflammatory bowel disease, and psoriasis, as well as psychological stress and depression.
- Variants in the TNF gene can influence the level of TNF production, which can have direct implications for inflammatory processes throughout the body and the brain.
4) Neurobiological Regulators and Resilience Factors
Genetic variations in crucial neurobiological regulators also govern resilience to stress. These include oxytocin, Brain-Derived Neurotrophic Factor (BDNF), and Neuropeptide Y (NPY). Oxytocin plays a role in regulating social behaviors and stress responses. BDNF is crucial for maintaining neuroplasticity and cognitive function under stress and NPY modulates anxiety and the physiological stress response. These molecules collectively impact our neural circuitry and psychological resilience, providing insights into individual differences in stress resilience and potential avenues for personalized biohacking strategies.
Oxytocin
Oxytocin is often called the "love hormone" because of its role in social bonding, maternal behaviors, and intimacy. It also exerts anxiolytic effects and influences social cognition and behavior.
- Genetic Influence: Variations in the oxytocin receptor gene (OXTR) have been associated with emotional regulation, social behavior, and stress responsiveness. Specific polymorphisms in OXTR can influence the binding efficiency and expression levels of oxytocin receptors, which may affect an individual's ability to handle stress and form social relationships.(28)
- Implications: In the context of resilience testing, assessing OXTR variants can provide insights into an individual's predisposition to social anxiety, empathy levels, and potential resilience in the face of stress, especially that which involves social dynamics.(29)
Brain-Derived Neurotrophic Factor (BDNF)
BDNF is a crucial protein involved in neuroplasticity, the brain's ability to reorganize and form new neural connections throughout life. It is critical for learning, memory, and the regeneration of neurons.(30)
- Genetic Variations: The BDNF gene variant Val66Met is one of the most studied polymorphisms. The Met allele has been associated with reduced activity-dependent secretion of BDNF, which might affect cognitive function and resilience to neurological and psychiatric disorders.(31)
- Implications: Testing for BDNF gene variants could help predict an individual's capacity for neuroplasticity in response to stress and could have implications for recovery from neurological insults or trauma.(32)
Image: An example page of the DNA Resilience test analysis.
Neuropeptide Y (NPY)
NPY is one of the most abundant peptides in the brain and is involved in regulating stress responses, anxiety and food intake. It is considered an endogenous anxiolytic agent.
- Genetic Associations: Polymorphisms in the NPY gene can lead to differences in NPY expression and secretion, potentially influencing an individual's stress resilience. Higher levels of NPY are generally protective against the effects of stress.
- Implications Genetic testing for NPY variants can potentially indicate an individual's baseline stress resilience and might predict their psychological response to chronic stress and trauma.(33)
The Role of Epigenetics in Modulating Stress Resilience
The field of epigenetics delves into a layer of complexity beyond the static DNA sequence. Epigenetic modifications consist of chemical changes to the DNA structure, such as methylation and histone modifications, which can affect how genes are expressed without altering the underlying genetic code. These changes are dynamic and responsive to environmental stimuli, including chronic stress. Exposure to prolonged stress can lead to epigenetic alterations that affect the functioning of genes involved in the stress response, potentially making it more difficult for individuals to handle new stressors effectively.(34-35)
Companies at the forefront of personalized medicine are now venturing into epigenetics, seeking to uncover how these modifications might contribute to an individual's capacity to withstand and bounce back from stress. By analyzing epigenetic markers, scientists can gain insights into the current state of gene expression profiles, which result from both genetic predisposition and environmental influences. Such tests can identify epigenetic changes in response to chronic stress, providing a snapshot of the molecular mechanisms contributing to an individual's stress response or lack thereof.
Furthermore, understanding these epigenetic changes opens the door to personalized interventions. Specific lifestyle changes, dietary adjustments, and therapeutic strategies might be recommended to reverse adverse epigenetic modifications. This personalized approach not only enhances an individual's resilience but also contributes to the broader understanding of how stress impacts our biological systems at an epigenetic level, which could lead to new treatments and preventive strategies for stress-related disorders. By mapping the epigenetic landscape of stress response, we can begin to paint a more comprehensive picture of the factors that contribute to our unique ability to cope with life's challenges.
The Benefits and Limitations of Resilience DNA Tests
These tests can offer individuals a better understanding of their innate resilience and stress response. Such knowledge could inform personalized strategies for managing stress and improving mental health. However, it is essential to approach these tests with carefulness:
- Complex Trait: Resilience is not determined by a single gene but is a complex trait influenced by many genes and environmental factors.
- Environmental Influence: Genetics does not work in isolation. Life experiences, support systems and lifestyle choices are significant in resilience.
- Predictive Power: While these tests can provide insights, they are not definitive predictors of an individual's ability to cope with life's challenges.
Conclusion
DNA tests related to resilience represent an intriguing frontier in understanding how our genetic makeup might influence the ability to handle stress and recover from adversity. While they can provide valuable insights, they should be seen as one piece of the giant puzzle that constitutes an individual's resilience. For anyone interested in these tests, it is recommended to consult with a healthcare provider or a genetic counselor to interpret the results within the broader context of their health and lifestyle.
- Get your Integral DNA test here!
- Book a consultation to interpret your lab and gene tests with Dr. Sovijärvi here.
Scientific references:
- Bobrow, M., & Grimbaldeston, A. H. (2000). Medical genetics, the human genome project and public health: Presented at the University of Liverpool, 9 December 1996 and accepted for publication on 17 February 2000. Journal of Epidemiology & Community Health, 54(9), 645-649.
- Cicchetti, D. (2010). Resilience under conditions of extreme stress: a multilevel perspective. World psychiatry, 9(3), 145.
- Luecken, L. J., & Gallo, L. C. (Eds.). (2008). Handbook of physiological research methods in health psychology. Sage.
- Southwick, S. M., Vythilingam, M., & Charney, D. S. (2005). The psychobiology of depression and resilience to stress: implications for prevention and treatment. Annu. Rev. Clin. Psychol., 1, 255-291.
- Michaud, M., Balardy, L., Moulis, G., Gaudin, C., Peyrot, C., Vellas, B., ... & Nourhashemi, F. (2013). Proinflammatory cytokines, aging, and age-related diseases. Journal of the American Medical Directors Association, 14(12), 877-882.
- Aguilera, G., Nikodemova, M., Wynn, P. C., & Catt, K. J. (2004). Corticotropin releasing hormone receptors: two decades later. Peptides, 25(3), 319-329.
- Subbannayya, T., Balakrishnan, L., Sudarshan, G., Advani, J., Kumar, S., Mahmood, R., ... & Prasad, T. K. (2013). An integrated map of corticotropin-releasing hormone signaling pathway. Journal of cell communication and signaling, 7, 295-300.
- Binder, E. B. (2009). The role of FKBP5, a co-chaperone of the glucocorticoid receptor in the pathogenesis and therapy of affective and anxiety disorders. Psychoneuroendocrinology, 34, S186-S195.
- Ising, M., Depping, A. M., Siebertz, A., Lucae, S., Unschuld, P. G., Kloiber, S., ... & Holsboer, F. (2008). Polymorphisms in the FKBP5 gene region modulate recovery from psychosocial stress in healthy controls. European Journal of Neuroscience, 28(2), 389-398.
- Vitellius, G., Trabado, S., Bouligand, J., Delemer, B., & Lombès, M. (2018, June). Pathophysiology of glucocorticoid signaling. In Annales d'endocrinologie (Vol. 79, No. 3, pp. 98-106). Elsevier Masson.
- Van West, D., Van Den Eede, F., Del-Favero, J., Souery, D., Norrback, K. F., Van Duijn, C., ... & Claes, S. (2006). Glucocorticoid receptor gene-based SNP analysis in patients with recurrent major depression. Neuropsychopharmacology, 31(3), 620-627.
- Schneider, K. K., Frings, C., Meyer, J., & Schote, A. B. (2016). The role of the glucocorticoid receptor gene (NR3C1) for the processing of aversive stimuli. Neuroscience Research, 107, 8-13.
- Azadmarzabadi, E., Haghighatfard, A., & Mohammadi, A. (2018). Low resilience to stress is associated with candidate gene expression alterations in the dopaminergic signalling pathway. Psychogeriatrics, 18(3), 190-201.
- Heinz, A., & Smolka, M. N. (2006). The effects of catechol O-methyltransferase genotype on brain activation elicited by affective stimuli and cognitive tasks. Reviews in the Neurosciences, 17(3), 359-368.
- Mier, D., Kirsch, P., & Meyer-Lindenberg, A. (2010). Neural substrates of pleiotropic action of genetic variation in COMT: a meta-analysis. Molecular psychiatry, 15(9), 918-927.
- Mustapic, M., Maihofer, A. X., Mahata, M., Chen, Y., Baker, D. G., O'Connor, D. T., & Nievergelt, C. M. (2014). The catecholamine biosynthetic enzyme dopamine β-hydroxylase (DBH): first genome-wide search positions trait-determining variants acting additively in the proximal promoter. Human molecular genetics, 23(23), 6375-6384.
- Vincent, S., & Robertson, D. (2002). The broader view: catecholamine abnormalities. Clinical Autonomic Research, 12, I44-I49.
- Hoenicka, J., Aragüés, M., Ponce, G., Rodríguez-Jiménez, R., Jiménez-Arriero, M. A., & Palomo, T. (2007). From dopaminergic genes to psychiatric disorders. Neurotoxicity research, 11, 61-71.
- Hill, S. Y., Hoffman, E. K., Zezza, N., Thalamuthu, A., Weeks, D. E., Matthews, A. G., & Mukhopadhyay, I. (2008). Dopaminergic mutations: Within‐family association and linkage in multiplex alcohol dependence families. American Journal of Medical Genetics Part B: Neuropsychiatric Genetics, 147(4), 517-526.
- He, Y., Martin, N., Zhu, G., & Liu, Y. (2018). Candidate genes for novelty-seeking: a meta-analysis of association studies of: DRD4: exon III and: COMT: Val158Met. Psychiatric genetics, 28(6), 97-109.
- Avula, R., Rand, A., Black, J. L., & O'kane, D. J. (2011). Simultaneous genotyping of multiple polymorphisms in human serotonin transporter gene and detection of novel allelic variants. Translational psychiatry, 1(8), e32-e32.
- Tivol, E. A., Shalish, C., Schuback, D. E., Hsu, Y. P., & Breakefield, X. O. (1996). Mutational analysis of the human MAOA gene. American journal of medical genetics, 67(1), 92-97.
- Waider, J., Araragi, N., Gutknecht, L., & Lesch, K. P. (2011). Tryptophan hydroxylase-2 (TPH2) in disorders of cognitive control and emotion regulation: a perspective. Psychoneuroendocrinology, 36(3), 393-405.
- Bauer, M. E., & Teixeira, A. L. (2021). Neuroinflammation in mood disorders: role of regulatory immune cells. Neuroimmunomodulation, 28(3), 99-107.
- Anderson, G., Kubera, M., Duda, W., Lasoń, W., Berk, M., & Maes, M. (2013). Increased IL-6 trans-signaling in depression: focus on the tryptophan catabolite pathway, melatonin and neuroprogression. Pharmacological Reports, 65(6), 1647-1654.
- Perry, B. I., Upthegrove, R., Kappelmann, N., Jones, P. B., Burgess, S., & Khandaker, G. M. (2021). Associations of immunological proteins/traits with schizophrenia, major depression and bipolar disorder: a bi-directional two-sample mendelian randomization study. Brain, behavior, and immunity, 97, 176-185.
- Bradley, J. (2008). TNF‐mediated inflammatory disease. The Journal of Pathology: A Journal of the Pathological Society of Great Britain and Ireland, 214(2), 149-160.
- Loth, E., Poline, J. B., Thyreau, B., Jia, T., Tao, C., Lourdusamy, A., ... & IMAGEN Consortium. (2014). Oxytocin receptor genotype modulates ventral striatal activity to social cues and response to stressful life events. Biological psychiatry, 76(5), 367-376.
- Myers, A. J., Williams, L., Gatt, J. M., McAuley-Clark, E. Z., Dobson-Stone, C., Schofield, P. R., & Nemeroff, C. B. (2014). Variation in the oxytocin receptor gene is associated with increased risk for anxiety, stress and depression in individuals with a history of exposure to early life stress. Journal of psychiatric research, 59, 93-100.
- Cowansage, K. K., LeDoux, J. E., & Monfils, M. H. (2010). Brain-derived neurotrophic factor: a dynamic gatekeeper of neural plasticity. Current molecular pharmacology, 3(1), 12-29.
- Chen, Z. Y., Jing, D., Bath, K. G., Ieraci, A., Khan, T., Siao, C. J., ... & Lee, F. S. (2006). Genetic variant BDNF (Val66Met) polymorphism alters anxiety-related behavior. science, 314(5796), 140-143.
- Phillips, C. (2017). Brain-derived neurotrophic factor, depression, and physical activity: making the neuroplastic connection. Neural plasticity, 2017.
- Schmeltzer, S. N., Herman, J. P., & Sah, R. (2016). Neuropeptide Y (NPY) and posttraumatic stress disorder (PTSD): a translational update. Experimental neurology, 284, 196-210.
- Lux, V. (2016, March). Epigenetic Programming in Psychobiological Development: Evidence for the Dual-Activation Theory and a Mediating Role of Early Life Stress. In Qatar Foundation Annual Research Conference Proceedings Volume 2016 Issue 1 (Vol. 2016, No. 1, p. HBOP3415). Hamad bin Khalifa University Press (HBKU Press).
- Chukwuma Sr, C. (2022). Epigenetics and its essence in understanding human growth, development and disease. J Med Res, 8(5), 165-172.